Calculating and Interpreting the QTc Interval in Children
The QTc interval on an electrocardiogram (ECG) represents the time it takes for the ventricles to depolarize and repolarize. A prolonged QTc interval is a significant risk factor for life-threatening arrhythmias, such as Torsades de Pointes. Correctly measuring and interpreting the QTc is a critical skill for paediatric trainees, as normal values in children vary by age and heart rate.
The QTc Interval
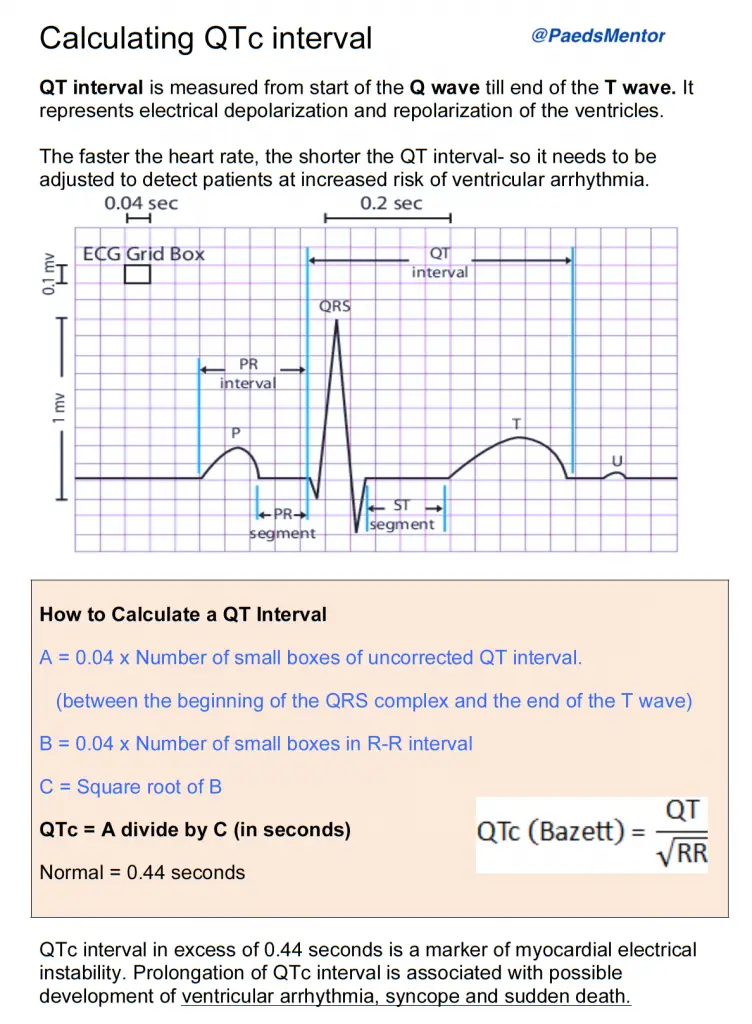
The QTc interval is the QT interval corrected for heart rate. A fast heart rate shortens the QT interval, while a slow heart rate lengthens it. To get an accurate QTc, a correction formula is used, with Bazett’s formula being the most common:
QTc = QT / √RR
QT Interval: Measure from the beginning of the QRS complex to the end of the T wave. The end of the T wave is the point where it returns to the baseline.
RR Interval: Measure the time between two consecutive R waves.
The QTc is considered prolonged in children if it is >450 ms in males and >460 ms in females. However, it’s also important to consider that a QTc can be prolonged in neonates and young infants, with values up to 490 ms sometimes considered within the normal range.
Clinical Implications
A prolonged QTc interval is a major red flag for Long QT Syndrome (LQTS), a genetic condition that predisposes to syncope and sudden cardiac death. Even if the QTc is within the normal range, a value that is borderline elevated in a child with a history of syncope, palpitations, or a family history of sudden death should prompt further investigation.
When to Calculate the QTc
The QTc should be calculated in the following clinical scenarios:
Syncope or Near-Syncope: Any child presenting with a brief loss of consciousness, especially without a clear trigger.
Seizures: A prolonged QTc can sometimes be misdiagnosed as a seizure.
Family History: A family history of sudden cardiac death, particularly in young relatives, or a known diagnosis of LQTS in a family member.
Pre-Surgical Clearance: In some cases, to rule out a pre-existing arrhythmia risk.
Medication Use: Before and during the use of drugs known to prolong the QT interval.
Medications That Prolong the QTc Interval
A large number of medications can prolong the QTc interval, increasing the risk of potentially fatal arrhythmias like Torsades de Pointes. This effect is often dose-dependent and can be exacerbated by other factors like electrolyte imbalances (hypokalaemia or hypomagnesaemia) or drug-drug interactions.
Antiarrhythmics: This is the most significant class.
Class Ia: Quinidine, Procainamide, Disopyramide.
Class Ic: Flecainide.
Class III: Amiodarone, Sotalol, Ibutilide, Dofetilide.
Antibiotics:
Macrolides: Erythromycin, Azithromycin, Clarithromycin.
Fluoroquinolones: Ciprofloxacin, Levofloxacin, Moxifloxacin.
Antifungals:
Azoles: Fluconazole, Itraconazole.
Antipsychotics:
Typical: Haloperidol, Chlorpromazine, Thioridazine.
Atypical: Quetiapine, Olanzapine, Risperidone.
Antidepressants:
Tricyclic Antidepressants (TCAs): Amitriptyline, Imipramine.
Selective Serotonin Reuptake Inhibitors (SSRIs): Citalopram, Escitalopram.
Antihistamines:
Older generation: Diphenhydramine.
Newer generation: Loratadine, Cetirizine (less common but possible in overdose).
Gastrointestinal Medications:
Prokinetics: Domperidone, Ondansetron.
Other:
Opiates: Methadone.
Antimalarials: Chloroquine, Hydroxychloroquine.
In a child on a medication known to prolong the QTc, the benefit of the drug must be weighed against the risk. In some cases, continuous cardiac monitoring or a cardiology referral may be necessary.
Pitfalls:
Measurement Errors: The most common pitfall is incorrectly measuring the QT interval, especially if the T wave is bifid or merges with a U wave. It is best to take an average of measurements from multiple leads (ideally Leads II and V5/V6).
Heart Rate Variation: The Bazett’s formula can be inaccurate at very high heart rates, so care must be taken.
