Microcephaly (Small Head Size)
A Structured Approach to Investigating Microcephaly in Children
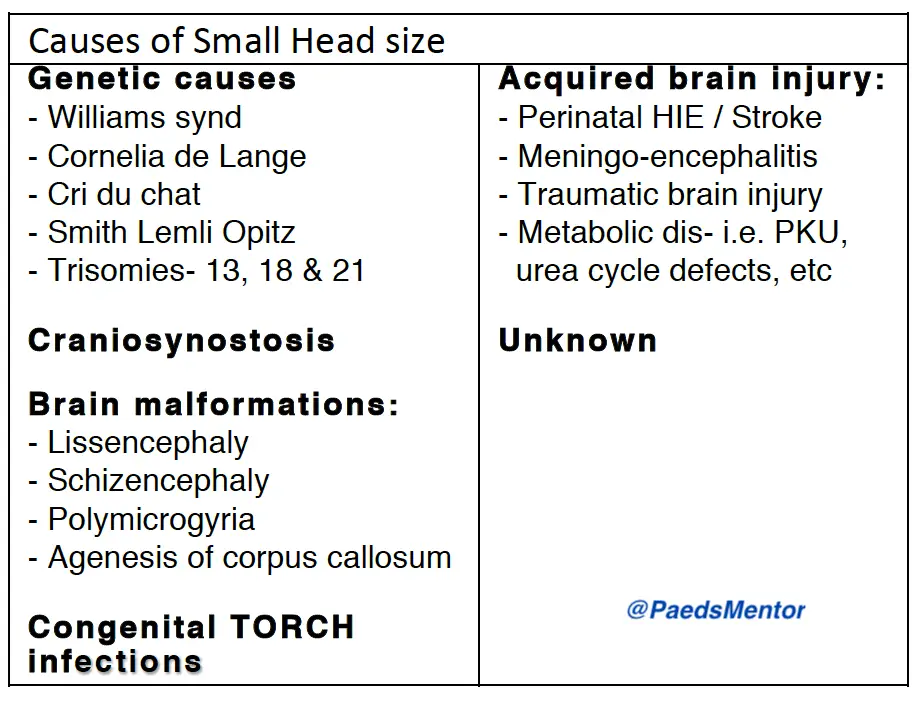
Microcephaly, a condition where a child’s head circumference is significantly smaller than average, requires a thorough investigation to identify the underlying cause. A systematic approach, starting with a detailed history and physical examination, is essential for guiding the right investigations and management plan.

History: Uncovering the Clues
A comprehensive history is the first step in determining the cause of a child’s microcephaly. The goal is to identify potential prenatal, perinatal, and postnatal factors.
Birth History: Ask about any significant issues around the time of birth, such as hypoxic-ischemic encephalopathy (HIE), neonatal seizures, or serious early-infancy illnesses like sepsis or meningitis.
Maternal and Pregnancy History: Inquire about any illnesses, infections (e.g., TORCH), or trauma during pregnancy. Also, ask about exposure to teratogens like alcohol, recreational drugs, or certain medications. Maternal malnutrition or placental insufficiency could lead to poor fetal growth and Intrauterine Growth Restriction (IUGR).
Developmental History: This is critical. Note any signs of developmental delay or regression of previously acquired skills. Ask about neurological symptoms like seizures, stiffness, feeding difficulties, or signs of raised intracranial pressure (ICP), such as vomiting or lethargy.
Family History: A detailed family history can reveal a genetic or neurodevelopmental disorder.
Physical and Neurological Examination
A focused physical examination provides key information about the child’s growth and neurological function.
Head Circumference and Shape: Plot the child’s head circumference on a growth chart over time to assess the trend. Examine the head shape for symmetry and feel for any abnormalities in the sutures or fontanelles.
Physical Features: Look for any dysmorphic features or malformations, especially around the eyes, palate, and spine, as these may point to an underlying genetic syndrome.
Neurological Examination: A full neurological exam is vital. Assess muscle tone for spasticity or dystonia and look for signs of autism spectrum disorder (ASD) or attention deficit hyperactivity disorder (ADHD), which can be associated with some causes of microcephaly.
Investigations: Choosing the Right Tests
The choice of investigations should be guided by the clinical findings from the history and examination.
Genetic Testing: A microarray is a key investigation, particularly if there are dysmorphic features, other congenital malformations, severe microcephaly, or a learning disability. It can help detect chromosomal abnormalities.
Neuroimaging: An MRI brain scan is the preferred imaging modality. It’s especially useful if there are neurological features such as seizures, spasticity, or developmental regression. A CT head scan may be considered if you suspect a condition like craniosynostosis or congenital infections (TORCH).
Infection Screening: A TORCH screen is performed if a congenital infection is suspected, especially in a young child.
Metabolic Tests: A selective neuro-metabolic workup may be considered if a metabolic disorder is suspected.
Management and Referrals: A Multi-Disciplinary Approach
Management is centered on supporting the child’s development and addressing any associated symptoms. This often requires a multi-disciplinary team.
Supportive Care: Provide therapy services as needed to support the child’s development. This can include physical, occupational, and speech therapy.
Symptom Management: Treat any associated symptoms like seizures or spasticity. Ensure the child receives extra support in school as required.
Referrals: Consider referrals to other specialists, including:
Ophthalmology: To check for vision problems.
Genetics: For further genetic counseling and testing.
Neurosurgery: If a condition like craniosynostosis is diagnosed.
