Paediatric Glasgow Coma Scale (pGCS)
Introduction: Why we need a modified GCS for children
The challenge of assessing consciousness in children: Unlike adults, children, especially infants and toddlers, cannot be assessed with the standard GCS criteria. They cannot “obey commands” or have an “oriented conversation.”
The purpose of pGCS: The Paediatric Glasgow Coma Scale (pGCS) is a modified version of the adult GCS designed to objectively and reliably assess a child’s level of consciousness. It is a critical tool for any healthcare professional caring for a sick child.
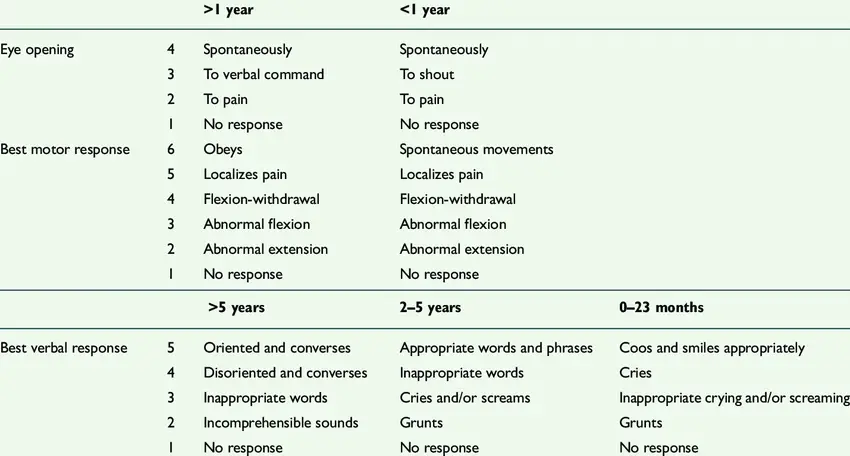
Key principle: The pGCS aims to evaluate consciousness across three domains: Eye opening, Verbal response, and Motor response, but with criteria adapted for different developmental stages.
The pGCS retains the same three categories as the adult scale (Eye, Verbal, Motor) and the same scoring range of 3 to 15. The core difference lies in the specific criteria used to assess verbal and motor responses, particularly for pre-verbal children.
When to use pGCS:
Following any head injury.
To monitor a child with an altered level of consciousness from any cause (e.g., meningitis, sepsis, seizure).
To track response to treatment.
Clinical Interpretation and Use in Practice
Total Score: The total score is the sum of the scores from the three components (E+V+M). The range is 3 to 15.
GCS 13-15: Mild impairment.
GCS 9-12: Moderate impairment.
GCS 3-8: Severe impairment. A GCS of ≤ 8 is a classic indication for airway protection and intubation.
The Importance of the Individual Scores: Trainees must be taught that the total score is a useful summary, but the individual scores are what provide the most useful clinical information. A drop in any one of the three components is a sign of neurological deterioration. For example, a child’s GCS might change from 15 (E4 V5 M6) to 13 (E4 V4 M5) because of a change in verbal response and motor response. This seemingly small drop is a critical sign that requires immediate action.
Important considerations and pitfalls:
“Best response”: Always score the best response a child can give. For example, if a child obeys commands on their right side but not their left, they get a score of 6 for motor.
“Not Testable”: If a component cannot be assessed (e.g., intubated child for verbal response, or a child with eye swelling), you should document “NT” (Not Testable) and cannot give a total score.
Painful stimulus: Trainees should be taught to apply painful stimuli judiciously and appropriately. A trapezius squeeze or supraorbital pressure is generally preferred over a sternal rub.
The child’s “normal”: Always get a history from the parents or caregivers to understand the child’s baseline level of consciousness and communication.
Don’t wait for a drop in GCS: Changes in other vital signs (e.g., bradycardia, irregular breathing, pupil changes) can be equally or more important indicators of a deteriorating neurological state. The GCS is a key part of the overall ABCDE assessment.
